-
-
Featured Care Areas

Cancer Care
While the incidence rates for cancer continue to rise globally, advances in medical technology are also evolving, and more people are surviving cancer today.
The fact is that with a well-rounded approach to cancer care, backed by strong professional and emotional support from experienced specialists, healthcare professionals and caregivers, many cancers can be effectively treated or managed.
Learn more about the different types of cancer, the importance of early cancer screening, cancer treatments and financial aids available, ways in which you may reduce your risk of cancer, and how to receive care and support in your cancer recovery journey.
What is cancer?
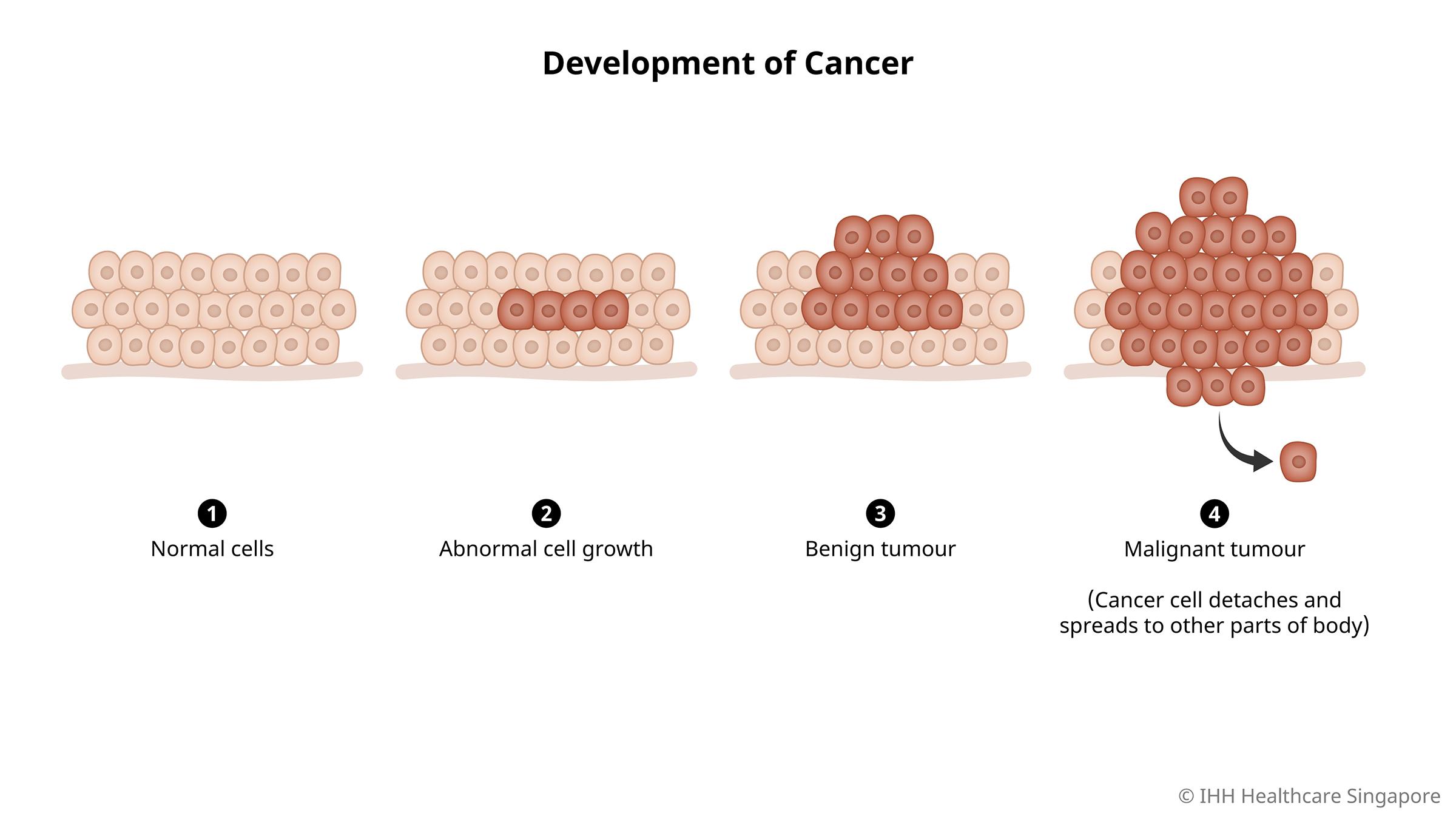
Cancer refers to a group of diseases characterised by the uncontrolled growth of abnormal cells in the body.
Cells are the basic building blocks of all living things, including the human body. As we age, our cells may experience changes, become damaged or die, and the body will normally generate new cells to replace them.
In some people, a genetic mutation or other causes will disrupt this process, and the cell becomes abnormal. As a result, it will divide and multiply uncontrollably, creating more abnormal cells, which will accumulate and form lumps known as tumours.
There are 2 types of tumours: benign tumours (non-cancerous and do not spread to other parts of the body) and malignant tumours (cancerous and can spread to other parts of the body).
What causes cancer?
Cancer can be caused by a combination of factors.
Non-modifiable factors include age, family history, and genetic mutations, which is the primary cause of cancer. This refers to changes to the DNA in your cells, which can be inherited. It can also occur after birth as a result of environmental factors.
Modifiable factors include diet, smoking, and exposure to carcinogens (cancer-causing agents), such as:
- Physical carcinogens (e.g. radiation and ultraviolet rays)
- Chemical carcinogens (e.g. cigarette smoke, asbestos, alcohol, air pollution, and contaminated food and drinking water)
- Biological carcinogens (e.g. viruses, bacteria, and parasites)
What are the symptoms of cancer?
Some general signs and symptoms experienced by people diagnosed with different types of cancer include:
- Fatigue
- Fever
- Unexplained weight loss
- Trouble with swallowing food
- Nausea and vomiting
- Swelling or lumps in the body
- Skin changes
- Persistent cough
- Persistent headaches
- Unusual bleeding or bruising
- Constipation or diarrhoea
- Pain when passing urine
- Vision or hearing problems
- Sores, bleeding or pain in the gums
However, symptoms vary according to the specific type of cancer, and may also be symptoms of many other more common, less life-threatening health conditions.
If you continue to experience more than one of the above symptoms for a long time, consult your doctor to detect any conditions early.
Did you know? Cancer is a leading cause of death in countries globally, accounting for approximately 10 million deaths in 2020.
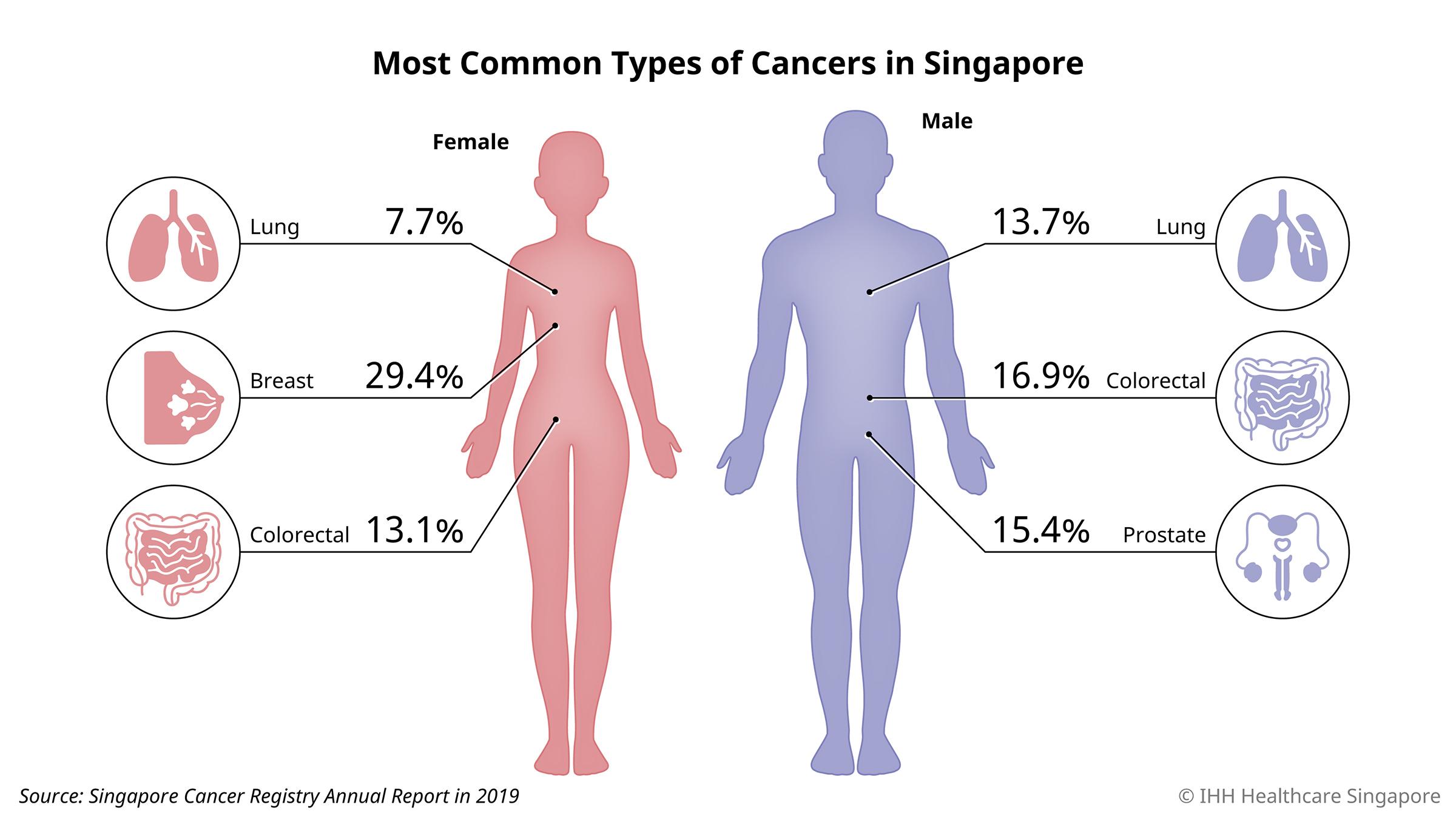
In Singapore, the most common cancers* occurring in men are colorectal cancer (16.9%), prostate cancer (15.4%) and lung cancer (13.7%). In women, it is breast cancer (29.4%), followed by colorectal cancer (13.1%) and lung cancer (7.7%).
Top cancers affecting men in Singapore
Colorectal cancer
This is the most common cancer affecting men in Singapore. Screening tests such as the Occult Blood Immunological (OBI) and a colonoscopy can help prevent it. Screening for colorectal cancer should begin at the age of 50 years. You can also consider going for a Lynch syndrome (hereditary colorectal cancer syndrome) clinical genetic test to determine your likelihood of getting the disease based on your family history.Prostate cancer
Prostate cancer is the 3rd most common cancer in Singapore, mainly affecting older men above 65 years of age. Early detection through prostate cancer screening can help reduce mortality.Lung cancer
This is the deadliest cancer affecting men in Singapore. People who are above 40 years old, are smokers, or have family members with a history of lung cancer, have the highest risk of getting lung cancer.
Top cancers affecting women in Singapore
Breast cancer
This is the most common cancer that afflicts women in Singapore. All women are at risk of breast cancer, and your risk increases if you are 50 years of age or older, and/or if your mother, sister or daughter has had breast cancer. The best way to protect yourself from breast cancer is to do a monthly breast self-examination or go for regular mammograms.You can also go for clinical hereditary breast and ovarian cancer syndrome genetic testing to gain critical insights into your risk of developing breast and ovarian cancer based on your family history or due to inherited genetic mutations.
Colorectal cancer
This is the second most common cancer affecting women in Singapore. Screening tests such as the Occult Blood Immunological (OBI) and a colonoscopy can help prevent it. Screening for colorectal cancer should begin at age 50 years.Lung cancer
This is the third most common cause of cancer death for women in Singapore. People who are above 40 years old, are smokers, or have family members with a history of lung cancer, have the highest risk.
*Source: Singapore Cancer Registry Annual Report in 2019
Can cancer be cured?
Many early stage cancers are treated with the aim to cure. While not all cancers may be cured completely, significant technological improvements in cancer treatments over the years means mortality rates are slightly decreasing, and survival rates are improving for many patients.
Usually, cancer treatment involves one of the following goals:
- To remove tumours completely
- To prevent recurrence or spread of the cancer
- To alleviate symptoms if all curative approaches have been considered
The most common approaches to treating cancer are surgery, radiotherapy, chemotherapy, targeted therapy and immunotherapy. The ideal treatment option is selected based on the location of the tumour, type and stage of the cancer, and the patient's personal health conditions and preferences.
Learn more about cancer treatments.
How can you prevent cancer?
While there is no proven way to prevent cancer, researchers are optimistic that regular health screening, personalised medicines, and good lifestyle habits can help to minimise the risk for the disease.
You can also reduce your risk by avoiding or stopping smoking, getting regular exercise, and eating a balanced and healthy diet. Some types of cancer may also be prevented through vaccinations.
Learn more about cancer prevention.
Cancer care at Mount Elizabeth
At Mount Elizabeth Hospitals, we have over 40 years of experience in caring for patients in need of diagnosis and treatment for different types of cancer. Our sophisticated and comprehensive suite of medical and surgical facilities, as well as rehabilitation and palliative services, ensure our patients receive the full spectrum of care.
We are one of the earliest private hospitals in Southeast Asia to introduce proton beam therapy, a new type of radiation therapy that uses protons instead of X-rays to treat advanced cancer. Through advanced procedures such as this, we have helped patients broaden their treatment options, with the goal of minimising the side effects of cancer treatment and increasing survival outcomes.
Our experienced cancer specialists at our hospitals and Parkway Cancer Centre are ready to take you under our wing with compassion and care.
Cancer care at Mount Elizabeth Hospitals is more affordable than you think. Your Integrated Shield Plan can help pay for the cost of your private hospital stay. Know your options.
Use our Hospital Bill Estimator to estimate your out-of-pocket expenses for common surgical procedures.
Our cancer specialists
50+
specialists
Mount Elizabeth is home to a robust and experienced team of medical oncologists and radiation oncologists. Get to know our cancer specialists and choose the right one for you.
Collapse All
Centres & Services
Mount Elizabeth Proton Therapy Centre
Radiation treatment that precisely delivers radiation to the tumour.

Mount Elizabeth Novena Centre for Genomic Health
Genetic testing that reveals disease-causing genetic mutations.
This page has been reviewed by our medical content reviewers.