Source: Shutterstock
What's Better? Natural Birth, or a C-Section?
Last updated: Thursday, March 18, 2021 | 6 min reading time
The arrival of your baby is an exciting event to look forward to and deciding on the birth plan can be a deeply personal one.
Congratulation, you are having a baby and it is now time to plan for the arrival of your bundle of joy. Your obstetrician may have offered you the choice of a natural (vaginal) delivery or an elective caesarean (C-section).
Deciding whether a natural or caesarean delivery is right for you is a question you should discuss with your doctor so that you know exactly what either option entails, and how your personal circumstances and medical history plays a part.
Here’s what you need to know before that conversation.
Before you make a decision…
While both modes of delivery are generally safe, they each carry a degree of risk which can vary mother to mother. A quick tip is to also check if your medical insurance plan covers complications from a natural and/or elective C-section delivery.
Here’s what to expect with each procedure and what the risks and complications may be.
What is a natural delivery?
A natural delivery happens when your baby is delivered naturally through your vagina.
What happens during natural childbirth?
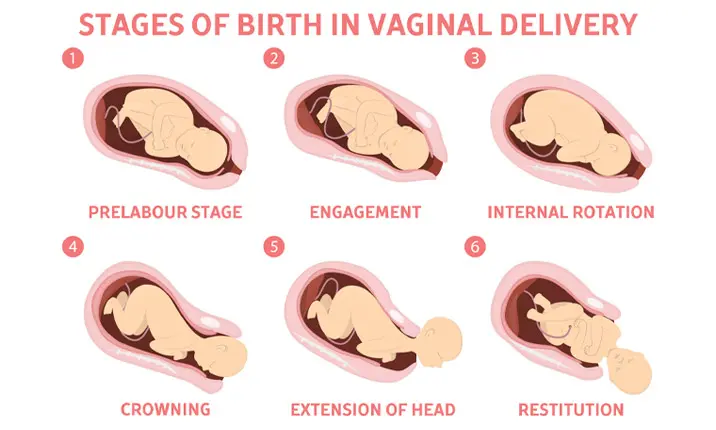
There are 3 stages of labour during vaginal childbirth. These stages are determined by the dilation (widening) of your cervix.
The contractions a pregnant woman experiences signal the start of labour. And the first stage of labour happens when her cervix has dilated to 10cm, and she will be asked to push. Stage 2 happens when the baby crowns, which is when the baby’s head is visible at the vagina opening. A final push should see the baby get delivered. In the final 3rd stage, the mother’s placenta is expelled.
How long does it take to recover from natural delivery?
Mothers who have had a natural vaginal delivery without any medical complications can expect to be discharged from hospital after 24 – 48 hours. As the body continues to heal for the next 3 – 6 weeks, vaginal bleeding may be experienced.
Are there risks in a natural delivery?
Not all vaginal births go as smoothly as planned. The delivery can involve one or all of the following.
- The doctor may advise labour induction for the mother and/or the baby’s safety.
- If the water bag has not broken and you are in labour, your doctor may perform an amniotomy (“breaking the water”) to rupture the amniotic membrane.
- The doctor may administer an intravenous synthetic hormone called oxytocin to hasten labour that is not progressing.
- Mothers may opt for an epidural (an anaesthetic injected into the epidural space around the spinal cord) to help manage the pain, although this may reduce the ability to feel the urge, or ability to push the baby out when the time comes.
- Besides an epidural, other medications such as Entonox (laughing) gas or a pethidine injection may be administered to manage the pain.
- The doctor may make a surgical incision called an episiotomy for the mother and/or baby’s safety as the baby’s head passes through the opening to your vagina. Stitches will be required after the delivery.
- If either mother or baby shows signs of distress in the course of deliver, the doctor may use forceps or vacuum extraction to assist in the safe delivery of the baby.
- If there are complications or risks to the health of the mother or baby during labour, the doctor may decide on an emergency C-section. While this can be disappointing for mothers who had planned for a vaginal delivery, it is necessary for the health and survival of both mother and child.
What is an elective C-section?
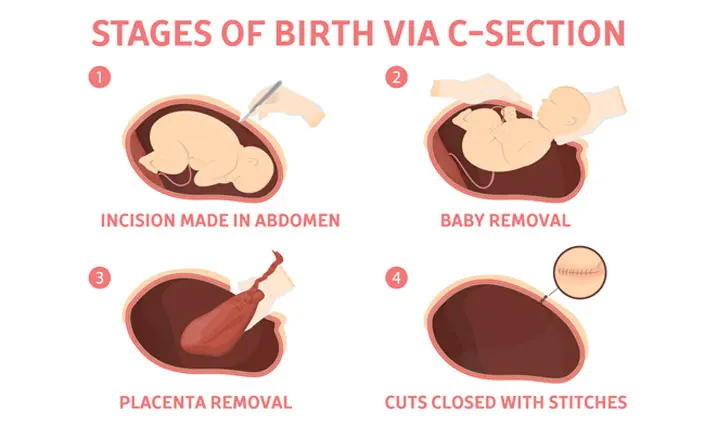
A C-section is a surgical procedure where your doctor makes an incision through your lower abdomen and uterus to deliver the baby. It can be done under regional (epidural or spinal block) or general anaesthetic. Mothers will remain awake for the former option.
An elective C-section is normally performed a week before the expected due date, or when the doctor notes that there might be a complication or health issues during pregnancy. However, mothers may request for their doctor to perform an elective C-section delivery after making an informed decision with the doctor.
While elective caesarean surgery is an option, it is not recommended because it is still a major surgery with risks of complications for both mother and child.
What are the advantages of an elective C-section?
Lower risk of:
- Urinary incontinence (inability to control the release of urine from the bladder)
- Pelvic organ prolapse (when the pelvic organs drop from their original position in the pelvis)
What are the disadvantages of an elective C-section?
- Risk of needing a C-section for future deliveries
- Risk of surgical complications
- Longer hospital stay (4 – 5 days) as compared to a natural delivery (2 – 3 days)
How long does it take to recover from a C-section?
You are required to be stay in hospital for 2 – 4 days after delivery and, in the first few weeks of recovery at home, the C-section scar may itch or cause pain that can be relieved with pain medication. Moving around and getting in and out of bed will be difficult and painful at the start.
Even though a mother had not gone through a vaginal delivery, they may still experience mild cramps, vaginal bleeding, or discharge for about 4 – 6 weeks. A follow-up appointment with the doctor post-birth will be necessary to review the wound; and at 6 weeks, a second follow-up appointment to assess recovery.
Are there other risks in a C-section?
Discuss the risks of a C-section with your doctor before making a decision on whether to undergo the procedure. Some of the possible risks include:
Risks to the mother
- Infection of, and pain and discharge from, the wound
- Infection of the womb lining or infection affecting other organs
- Excessive bleeding which may require a blood transfusion or further surgery to stop the bleeding in serious cases
- Blood clotting, which could be very dangerous if it travels to the lungs (pulmonary embolism)
- Damage to your bladder or the tubes that connect the kidneys and bladder or bowel, which may require further surgery
- The need for a hysterectomy (surgery to remove the womb) if there are serious complications such as life-threatening bleeding.
Risks to the baby
- The baby may be cut accidentally as the womb is opened. Such wounds are usually superficial and heal well.
- There may be a chance of the baby experiencing breathing difficulties and may need to be monitored longer in hospital.
Risks to future pregnancies
Many women who had a C-section can go on to deliver their next baby safely by vaginal delivery. However, there are always risks of complications in future pregnancies. These include:
- the scar in the womb opening up
- the placenta being abnormally attached to the wall of the womb, leading to pregnancy complications
Discuss each type of delivery with your doctor so an informed decision can be made. Weigh up the pros and cons for the health of both mother and baby as it may affect future plans to have more children. Remember, just because an elective C-section is an option, it may not be the best choice for mother and child.
C-Section vs. Natural Birth: Which Is Right for You? Retrieved 10/11/2020 from https://www.healthline.com/health/pregnancy/c-section-vs-natural-birth-2
Reasons for a C-Section: Medical, Personal, or Other. Retrieved 10/11/2020 from https://www.healthline.com/health/pregnancy/c-section-reasons#What-are-the-medical-reasons-for-a-C-section?
Is a Planned C-Section Right for Me? Retrieved 10/11/2020 from https://www.webmd.com/baby/c-section-cesarean#1
Risks. Caesarian Section. Retrieved 10/11/2020 from https://www.nhs.uk/conditions/caesarean-section/risks/
Reasons for a C-Section: Medical, Personal, or Other. Retrieved 10/11/2020 from https://www.healthline.com/health/pregnancy/c-section-reasons#What-are-the-medical-reasons-for-a-C-section?
Is a Planned C-Section Right for Me? Retrieved 10/11/2020 from https://www.webmd.com/baby/c-section-cesarean#1
Risks. Caesarian Section. Retrieved 10/11/2020 from https://www.nhs.uk/conditions/caesarean-section/risks/
 Brain & Spine Care
Brain & Spine Care