Source: Shutterstock
How to Prevent Breast Cancer
Last updated: Thursday, April 22, 2021 | 4 min reading time
More than 3,000 cases of breast cancer are diagnosed in Singapore every year, and in 2020, some 900 women died from the disease.
Looking at these statistics, it is unsurprising that breast cancer is the No. 1 cancer diagnosed among women in Singapore, and it accounts for 32% of all female cancers. While these figures are alarming, there are steps you can take to reduce your risk of developing breast cancer, and overcome the disease with early detection and treatment.
Who is at risk of developing breast cancer?
Women over 40 years of age have a greater chance of developing breast cancer. Here are some other risks to be aware of.
Your family history – Having a family history of breast cancer increases your risk of the disease. That risk doubles if a first degree relative, such as your mother or sister, has breast cancer, because 5 – 10% of breast cancers are hereditary. Patients with an inherited genetic mutation causing cancer usually have multiple first and second-degree relatives with breast, or other, cancers related to the mutation. Common genetic mutations like BRCA 1 and 2 raises the lifetime risk of developing breast cancer to between 60 – 80%.
Your reproductive history – If you delayed having children to beyond age 35, your menses started before you were 12, or you entered menopause late after age 55, you will have had a more prolonged exposure to oestrogen than the general population, which increases your breast cancer risk.
Your lifestyle – Your weight and dietary habits also play a part in increasing your risk. Excess weight and lack of exercise, especially post menopause, can increase the risk of breast cancer. Similarly, a diet high in red meat, animal fat and alcohol can increase that risk. Conversely, soy products, omega 3 oil from fish and a diet rich selenium and vitamins A, C and E can help protect against the disease.
Your exposure to hormones – Prolonged oral contraceptive or Hormone Replacement Therapy (HRT) use increases the risk of breast cancer. When considering hormone therapy, discuss the risks and benefits with your doctor.
It’s not just a disease for older women
From 2011 to 2015, 4,616 women below age 54 in Singapore were diagnosed with breast cancer. The rise in breast cancer cases among pre-menopausal women may be attributed to today’s urban lifestyles, where women tend to delay having children into their 30s, and generally have fewer children. An unhealthy and sedentary lifestyle also plays a factor along with smoking and increased alcohol consumption.
How to reduce your risk of breast cancer
With 1 in 13 women in Singapore likely to be diagnosed with breast cancer in their lifetime, all women should be aware of measures to decrease their risk of breast cancer.
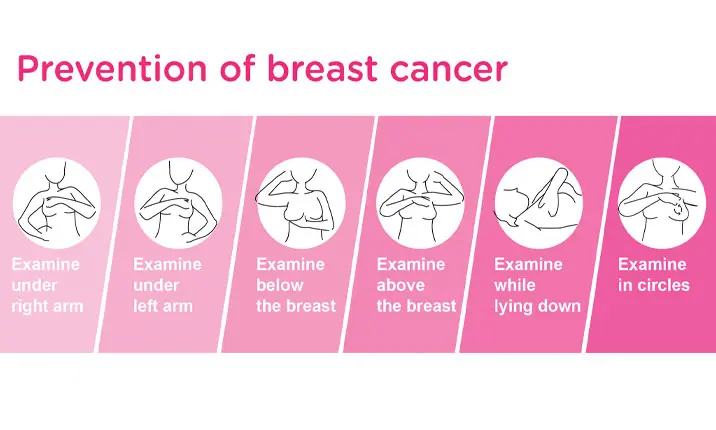
Breast self-examination – Check your breasts monthly (between Day 7 to Day 10 of your menstrual cycle) for any changes. If you notice changes such as dimpling of the skin or a change in the appearance of your nipples, get this checked with your doctor.
Breast cancer screening – Start screening for breast cancer with annual mammograms once you reach age 40, or 10 years earlier than the age of the youngest afflicted family member in the family. This is currently the most reliable screening tool for breast cancer as it can detect the presence of cancerous lumps even before they can be felt during a breast self-examination.
Healthy lifestyle choices – Maintain a healthy weight, consume a nutritious diet, reduce your intake of alcohol and don’t smoke. Women who observe a Mediterranean diet supplemented with extra-virgin olive oil and mixed nuts seem to have increased success at staving off breast cancer. This diet is primarily plant-based and includes healthy fats such as olive oil instead of butter, and fish instead of red meat.
Genetic counselling and genetic testing – If you have multiple family members with breast or ovarian cancer, you may consider genetic counselling to assess your breast cancer risk. Women at high risk of breast cancer need to discuss further preventive measures with their breast surgeon or oncologist. Options include hormonal therapy or prophylactic mastectomies.
Preventive prophylactic mastectomies – Women at high risk of developing breast cancer may opt to undergo bilateral mastectomies, or the removal of both breasts, before any cancer is detected. This results in a 90 – 95% reduction in the risk of breast cancer occurring. Bilateral breast reconstruction is commonly performed at the same time, so that the patient suffers the least socio-psychological stress.
Diagnosing breast cancer
Mammography is not only used in screening for breast cancer but aids in its diagnosis as well. It is a type of low-dose X-ray that delivers images of the tissue within the breast. If abnormal findings are detected, further additional images of the breast may be required to give a clearer assessment of the area of interest.
A mammogram can help detect calcifications and masses in the breast but can’t prove these changes are due to cancer. Your doctor will order further tests such as a biopsy to make a confirmed diagnosis.
Mammography has improved over the years and 3D mammograms now lead to fewer call backs for further imaging and are better at detecting changes, even in dense breasts.
If you are a woman over 40 years of age, or are at higher risk of developing breast cancer, go for a regular mammogram every year. It’s a simple procedure that may just save your life.
Mount Elizabeth Hospitals offer a one-stop solution for all your breast screening, assessment and diagnostic needs at the Mount Elizabeth Breast Care Centre.
Our dedicated team of surgeons, radiologists, nurses and allied health professionals work closely to provide comprehensive and personalised care to support you through your breast health journey.
Retrieved 18 March 2021 from https://www.mavensurgery.com.sg/breast-surgery.html
Retrieved 18 March 2021 from https://www.singhealth.com.sg/news/patient-care/more-women-in-singapore-diagnosed-with-advanced-breast-cancer-younger-women-not-spared-disease
Retrieved 18 March 2021 from https://www.nccs.com.sg/patient-care/cancer-types/cancer-statistics
Retrieved 18 March 2021 from https://www.singaporecancersociety.org.sg/learn-about-cancer/cancer-basics/common-types-of-cancer-in-singapore.html
Retrieved 18 March 2021 from https://www.medicalnewstoday.com/articles/37136#symptoms
Retrieved 18 March 2021 from https://www.mayoclinic.org/healthy-lifestyle/womens-health/in-depth/breast-cancer-prevention/art-20044676
Retrieved 18 March 2021 from https://www.singaporecancersociety.org.sg/get-screened/breast-cancer/mammogram.html
Retrieved 18 March 2021 from https://www.cancer.org/cancer/breast-cancer/screening-tests-and-early-detection/mammograms/mammogram-basics.html
Retrieved 18 March 2021 from https://www.singhealth.com.sg/news/patient-care/more-women-in-singapore-diagnosed-with-advanced-breast-cancer-younger-women-not-spared-disease
Retrieved 18 March 2021 from https://www.nccs.com.sg/patient-care/cancer-types/cancer-statistics
Retrieved 18 March 2021 from https://www.singaporecancersociety.org.sg/learn-about-cancer/cancer-basics/common-types-of-cancer-in-singapore.html
Retrieved 18 March 2021 from https://www.medicalnewstoday.com/articles/37136#symptoms
Retrieved 18 March 2021 from https://www.mayoclinic.org/healthy-lifestyle/womens-health/in-depth/breast-cancer-prevention/art-20044676
Retrieved 18 March 2021 from https://www.singaporecancersociety.org.sg/get-screened/breast-cancer/mammogram.html
Retrieved 18 March 2021 from https://www.cancer.org/cancer/breast-cancer/screening-tests-and-early-detection/mammograms/mammogram-basics.html
 Brain & Spine Care
Brain & Spine Care