Source: Shutterstock
What to Expect at Your First Visit to the Gynae
Last updated: Monday, February 1, 2021 | 5 min reading time
During a routine gynaecological visit, your gynae might perform different screening exams depending on your age and disease risk to assess your health.
Women's health screening
Screening tests are used for early detection and prevention. For women, these include annual Pap smears, mammogram and bone density test, as well as other tests for diseases that you might be at risk for. These screening tests are crucial for spotting illnesses even before any symptoms are present. Early detection and treatment in turn often result in fewer complications and better outcomes.
Consult your doctor to discuss about tests that may benefit you.
When to see a gynaecologist
Women are advised to visit a gynaecologist annually for a routine checkup and at any time they have any concerning symptoms. These include pain in the pelvis, vulva or vagina and abnormal bleeding from the uterus.
Some of the issues and conditions that are generally handled by a gynaecologist are:
- Those relating to pregnancy, fertility, menstruation and menopause
- Family planning
- Sexually transmitted diseases
- Polycystic ovary syndrome
- Urinary and faecal incontinence
- Conditions involving the breasts and reproductive organs
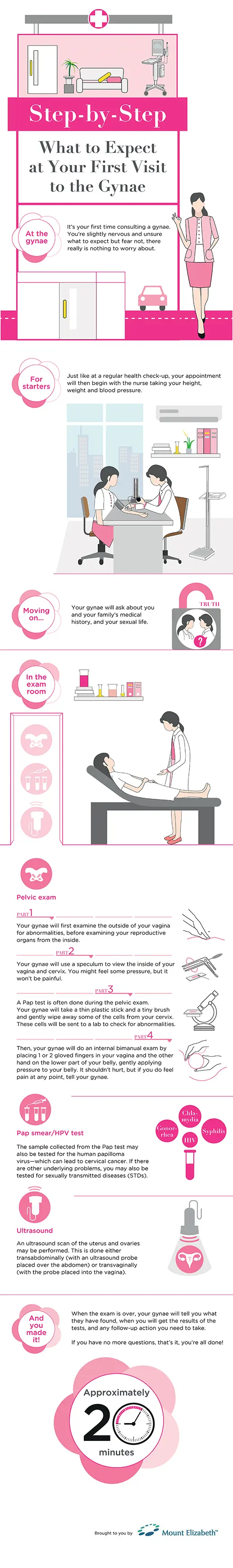
What to expect at your first gynaecology examination
It's your first time consulting a gynae. You're slightly nervous and unsure what to expect but fear not, there really is nothing to worry about.
Just like at a regular health check-up, your appointment will begin with the nurse taking your height, weight and blood pressure.
Your gynae will ask about you and your family's medical history, and your sexual life.
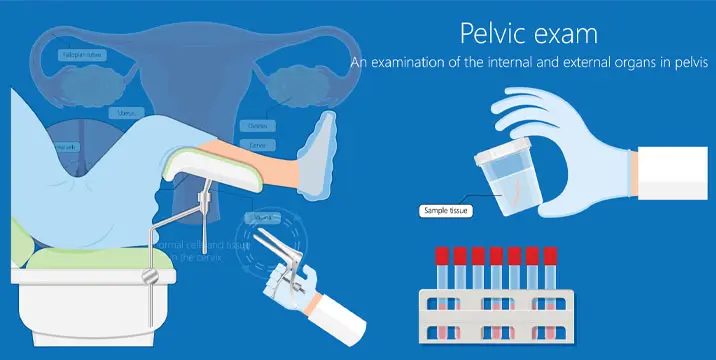
Pelvic exam
Part 1: Your gynae will first examine the outside of your vagina for abnormalities, before examining your reproductive organs from the inside.
Part 2: Your gynae will use a speculum – a device that holds the vagina open – to view the inside of your vagina and cervix. You might feel some pressure, but it won't be painful.
Part 3: A Pap test is often done during the pelvic exam. Your gynae will take a thin plastic stick and a tiny brush and gently wipe away some of the cells from your cervix. Those cells will be sent to a lab and checked for abnormalities.
Part 4: Then, your gynae will do an internal bimanual exam by placing 1 or 2 gloved fingers in your vagina and the other hand on the lower part of your belly, gently applying pressure to your belly. It shouldn't hurt, but if you do feel pain at any point, tell your gynae.
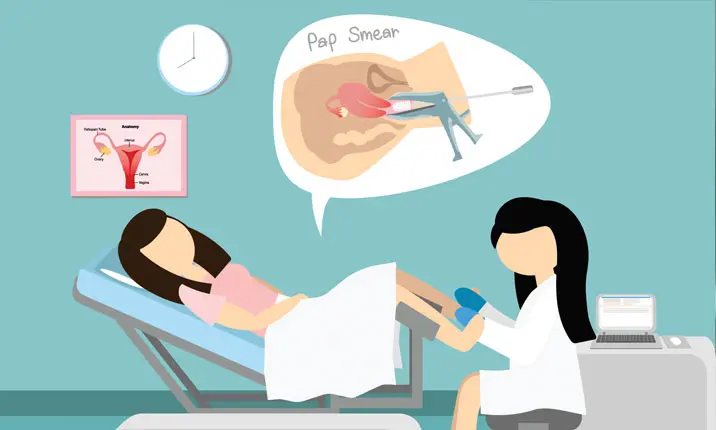
Pap smear / HPV test
The sample collected from the Pap test may also be tested for the human papilloma virus – which can lead to cervical cancer. If there are other underlying problems, you may also be tested for sexually transmitted diseases (STDs).
Who should have a Pap smear test
Women between the ages of 21 and 65 should undergo a Pap smear test every 3 years. As not all cervical cancers are from HPV infections (which are sexually transmitted), women who are not sexually active are also recommended to have a Pap smear every 3 years.
The following risk factors may warrant more-frequent Pap smear tests:
- A cervical cancer diagnosis or a Pap smear that showed precancerous cells
- Exposure to diethylstilboestrol (a synthetic form of oestrogen) before birth
- HIV infection
- Weakened immune system due to organ transplant, chemotherapy or chronic corticosteroid use
- A history of smoking
Preparing for a Pap smear test
Try to avoid having sexual intercourse, douching or using spermicidal products the day before your test. It is best to avoid scheduling your test when you're menstruating as the results may be less accurate. Pap smears are safe in the first 24 weeks of pregnancy. After that, you may experience more pain during the procedure. It is also advisable to wait until 12 weeks after giving birth to increase the accuracy of your test results.
What happens during a Pap smear test
A Pap smear test is very quick. During the procedure, you will lie on your back on an examination table with your legs spread and your feet resting in supports called stirrups.
Your doctor will slowly insert a device called a speculum into your vagina. This is to keep the vaginal walls open and gives access to the cervix. Your doctor will then scrape a small sample of cells from your cervix using a spatula and a brush. This might be a bit uncomfortable. You may fee a slight push and irritation during the brief scraping.
The sample of cervical cells will then be sent to a lab to be tested for any abnormal cells. After the test, you may feel mild discomfort, slight cramping or very light bleeding.
Tell your doctor if any of these symptoms persist for more than one day.
What do Pap smear results mean
A Pap smear test result may either be normal or abnormal.
- Normal Pap smear results are also called negative results. This means no abnormal cells were identified and you can have your next Pap smear after 3 years unless any symptoms develop.
- Abnormal Pap smear results mean that there are abnormal cells on your cervix that could be precancerous. There are several types of abnormal cells and depending on the type you have, your doctor may recommend you increase the frequency of your Pap smears or undergo a procedure called colposcopy to get a closer look at your cervical tissues.
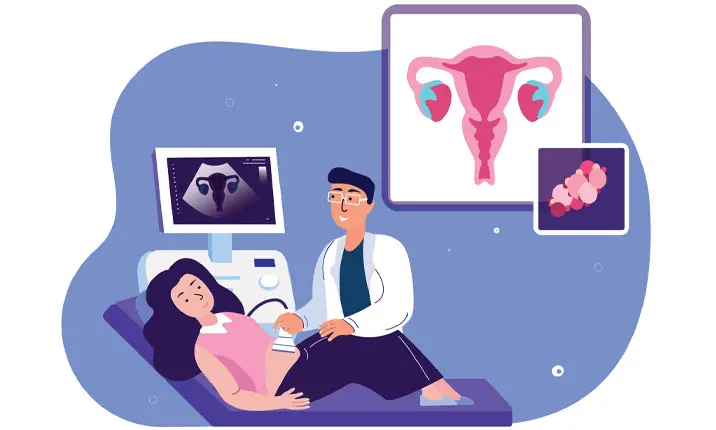
Ultrasound
An ultrasound scan of the uterus and ovaries may be performed. This is done either transabdominally (with an ultrasound probe placed over the abdomen) or transvaginally (with the probe placed into the vagina).
Who should have a pelvic ultrasound
A pelvic ultrasound may be for you if your doctor suspects any of the following:
- Abnormal size, shape or position of your uterus or ovaries
- Cancer in your ovaries, uterus or bladder
- Growths such as noncancerous tumours, fibroids or cysts
- Abnormal bleeding or pain
- Fertility problems
- Pregnancy
- Pelvic inflammatory disease
Preparing for a pelvic ultrasound
If you are undergoing a transabdominal ultrasound, you will need to drink about 1 litre of water so your bladder will be full, which makes your organs show up more clearly during the procedure.
For a transvaginal ultrasound, your bladder will need to be empty. Use a bathroom before the test.
You will be asked to remove and jewelry, clothes or other objects that may interfere with the scan. A gown will be provided if you are asked to remove your clothes.
What happens during a pelvic ultrasound
During a transabdominal ultrasound, you will lie on your back on an examination table. A gel-like substance will be applied on your abdomen. Your doctor will press a tool (transducer) against your skin and move it around over the area being examined. Images of structures will be seen on a computer screen. Once the procedure is completed, the gel will be removed and you may empty your bladder.
For a transvaginal ultrasound, you will lie on an examination table, with your feet and legs supported as for a pelvic examination. A long, thin tool (transvaginal transducer) that is covered with a plastic or latex sheath and lubricated will be inserted into your vagina. The transducer will be gently turned and angled to bring the areas for examination into focus. You may feel some discomfort as the transducer is moved. Images of structures will be seen on a computer screen.
What happens after a pelvic ultrasound
After a pelvic ultrasound, a radiologist will analyse the ultrasound images and send a report to your doctor. Your doctor will explain the test results and may recommend further tests if there are any concerns.
And you made it!
When the exam is over, your gynae will tell you what they have found, when you will get the results of the tests, and any follow-up action you need to take. Use your appointment as an opportunity to ask questions. Ask about periods, sex, or whatever you want to know about your reproductive health. You don't have to be shy or embarrassed about asking – your gynae has heard it all!
If you have no more questions, that's it, you're all done!
Total time taken: Approximately 20 minutes.
Gynaecologists: When to Visit and What to Expect. (2017, August 29) Retrieved December 04, 2020, from https://www.medicalnewstoday.com/articles/288354
Pap Smear (Pap Test): What to Expect. (2020, February 26) Retrieved December 04, 2020, from https://www.healthline.com/health/pap-smear#pap-smear-frequency
Pap Smear (2020, June 25) Retrieved December 04, 2020, from https://www.mayoclinic.org/tests-procedures/pap-smear/about/pac-20394841
What Is a Pelvic Ultrasound? (2019, January 30) Retrieved December 04, 2020, from https://www.webmd.com/women/what-is-a-pelvic-ultrasound
Pelvic Ultrasound. (n.d) Retrieved December 04, 2020, from https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/pelvic-ultrasound
Pap Smear (Pap Test): What to Expect. (2020, February 26) Retrieved December 04, 2020, from https://www.healthline.com/health/pap-smear#pap-smear-frequency
Pap Smear (2020, June 25) Retrieved December 04, 2020, from https://www.mayoclinic.org/tests-procedures/pap-smear/about/pac-20394841
What Is a Pelvic Ultrasound? (2019, January 30) Retrieved December 04, 2020, from https://www.webmd.com/women/what-is-a-pelvic-ultrasound
Pelvic Ultrasound. (n.d) Retrieved December 04, 2020, from https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/pelvic-ultrasound
 Brain & Spine Care
Brain & Spine Care