Source: Shutterstock
Discover the Possible Causes of Back & Leg Pain
Last updated: Thursday, January 28, 2021 | 3 min reading time
Back pain that spreads down your legs is more common than you might think. Dr Mashfiqul Siddiqui, orthopaedic surgeon at Mount Elizabeth Hospital, explains the possible causes and treatments for back pain.
The sciatic nerve is the largest single nerve in the body. It starts in the lower back, running through each buttock and down the back of each leg, with sections spreading into your thighs, calves, feet and toes.
What is sciatica?
Sciatica refers to pain caused by compression of the sciatic nerve, resulting in irritation or inflammation. When this happens, it's common to experience pain, a burning or tingling sensation, or weakness and numbness in your legs. This pain will follow the same path as the nerve, beginning in the lower back, down into the buttocks and into the legs.
Sciatica can result in difficulty in sitting or walking. Sciatica can affect either leg, but usually only affects one side and in most cases, resolves without the need for invasive procedures.
Causes of sciatica
Sciatica is usually the result of a herniated disc in the spine. Other causes of similar leg symptoms can result from compression of the spinal nerves. This is called spinal stenosis. Direct damage to the nerve is rare.
Risk factors for sciatica from a herniated disc include obesity, prolonged sitting and carrying of heavy loads. With increasing age, the space in the spine for the nerves can become smaller resulting in compression of the nerves from spinal stenosis.
Your risk for sciatica increases with age and obesity, because ageing as well as excessive weight or stress on the spine can lead to spinal changes. Some daily habits can also make it more likely to develop, such as prolonged periods of sitting or inactivity, or regularly carrying heavy loads. Some conditions also play a role, such as diabetes which may lead to nerve damage and osteoarthritis which contributes to spinal damage.
Symptoms of Sciatica
Sciatica pain typically radiates from the lower back, into the buttocks and down the back of the legs. The sensation can vary from person to person, ranging from a mild ache to sharp pain that burns or feels like an electric shock.
The pain usually feels more severe in the legs compared to the lower back, and some people may find that the pain comes and goes, while others find that the pain is always present.
Another possible cause of lower back pain is what's normally called a pinched nerve, medically known as radiculopathy.
What is a pinched nerve (radiculopathy)?
Radiculopathy is a general term referring to a compressed or irritated nerve, which can occur anywhere along the spinal column. Depending on its location, these can be described as cervical (neck), thoracic (upper back) or lumbar (lower back) radiculopathy.
What causes radiculopathy?
According to Dr Mashfiqul, there are many things that can put pressure on your nerves and result in pain.
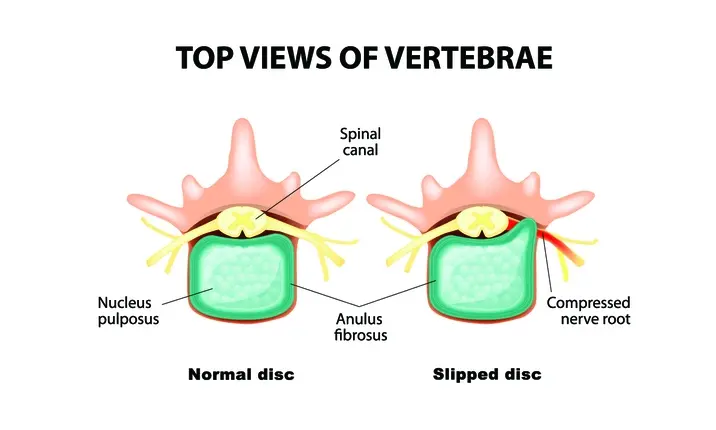
Slipped disc
"Often, the problem lies in the nerves that are in the spine," he says. "In younger patients, the cause of nerve compression is usually a slipped disc (when one of the padded discs between your spinal bones protrudes backwards). In these patients, the pain usually goes down one leg, correlating with whichever nerve is compressed."
"In older patients, sometimes the spinal bone (vertebra) itself can slip forward, which puts pressure on more than one nerve. These patients may complain of pain going down both calves when they walk, which is relieved by rest."
When any nerve is compressed, it's not unusual to feel tingling or numbness. Occasionally, the leg muscles themselves may weaken. In more severe cases, problems with bladder or bowel dysfunction may occur.
A malfunctioning nerve may also result in similar symptoms, although this is less common.
Symptoms of radiculopathy
Radiculopathy can cause a broad range of symptoms, which include:
- sharp pain beginning in the back and extending to the foot
- sharp pain beginning in the back of the neck extending to the shoulder, arm or hand
- sharp pain with sitting or coughing
- numbness or weakness in the arm, leg and foot
- numbness or tingling in the arm or leg
- worsening pain with movement of the neck or head
When should I go see a doctor?
If you have symptoms of an irritated nerve that are not getting better over time, make sure to visit your doctor for a proper diagnosis. Seek a consultation as soon as possible if your arms or legs feel weak or numb.
If you are struggling to pass urine, go to the emergency department and seek medical advice immediately.
How is radiculopathy diagnosed?
MRI (magnetic resonance imaging)
Often, your doctor will recommend an MRI (magnetic resonance imaging) body scan before making a diagnosis. You'll need to lie down so the machine can scan your neck and/or back. This will help your doctor to identify exactly which nerve, or nerves, are compressed in your spine, as well as where they are located and how severe the problem is.
X-Ray
You may also need to have an x-ray. This is carried out in a standing position, which makes it easier for your doctor to see the alignment of your spine.
Nerve conduction test
If your doctor suspects the nerves themselves are malfunctioning without any compression in the spine, they may also do a nerve conduction test, which measures how fast electrical impulses travel through your nerves. This involves applying small electrodes - one which sends a mild electrical pulse, and the other records the resulting nerve activity.
How is radiculopathy treated?
Treatment really depends on what's causing the pain in your arms or legs.
"Common problems such as slipped disc can often be managed with medication and physiotherapy, with simple exercises to relieve pain and improve mobility," explains Dr Mashfiqul. "Sometimes, steroid injections may also help. If problems persist, your doctor may suggest a microdiscectomy, a minimally invasive surgery to remove the disc through a small cut in the back."
"If one of your bones has moved out of place and is putting pressure on a nerve (known as spondylolisthesis), physical therapy, medications and heat/ice therapy can all help. But if the pain is severe or ongoing, a spinal fusion surgery is generally effective. This joins 2 or more bones together using screws and bone grafts to keep them from shifting."
Physiotherapy
A physiotherapist can help to recommend exercises aimed at:
- stretching, to improve flexibility and relieve tight muscles in the lower back and hips, thighs, pelvis and buttocks
- strengthening core muscles to help support good posture
- posture training to improve body alignment and reduce undue stress on the spine
Steroid injections
Steroid injections, also known as injectable corticosteroids, may be recommended to help relieve pain and inflammation. These are injected near the location of the pinched nerves. Injectable corticosteroids are associated may have some side effects or contraindications so be sure to speak to your doctor about any existing healthcare conditions you may have.
Microdiscectomy
A microdiscectomy is a minimally invasive surgical procedure to relieve pressure on the spinal nerves by removing parts of a herniated disc. It is an alternative to conventional open surgery which involves a larger incision and a longer recovery period. With microdiscectomy, small incisions are made and the procedure performed using a microscope. Most people can return home on the same day or after a short period of observation.
Spinal fusion surgery
Following the removal of a damaged or herniated disc, spinal fusion surgery may sometimes be recommended to help stabilise your spine. In this procedure, your surgeon will place bone and/or synthetic material between two vertebrae, with the addition of metal screws and rods to hold everything together.
If you are experience ongoing back and leg pain or neck and arm pain, it is best to seek a proper diagnosis before considering your options. However, even if you are diagnosed with a nerve-related condition, there is no need to be overly concerned. Once your condition is properly diagnosed, your doctor will recommend a suitable treatment after evaluating your symptoms, possible causes, medical history and overall health.
 Brain & Spine Care
Brain & Spine Care