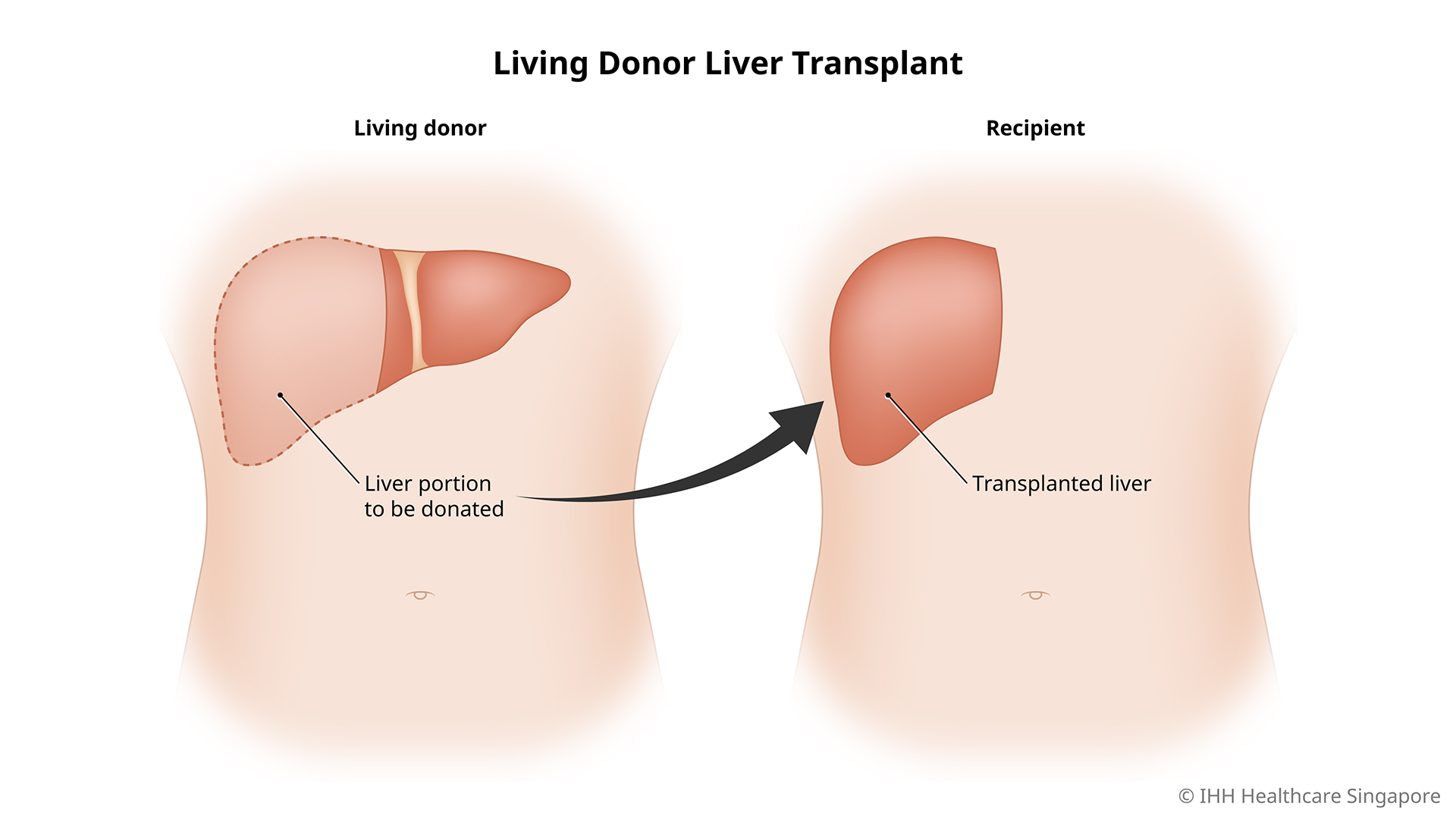
What can you expect in an LDLT?
If you're receiving a liver transplant from a living donor, your surgery will be scheduled in advance.
Estimated duration
A liver transplant usually takes between 6 – 12 hours.
During the procedure
During the transplant, the surgeon will make an incision over your upper abdomen to remove your liver and replace it with the donor liver graft. The specific part of the liver donated depends on the size of the donor liver and your needs.
Next, the surgeon will connect the blood vessels and bile ducts to the new liver to restore blood flow. The incision will be closed once the vital structures are anastomosed (joined) and working well.
After the procedure
After your liver transplant, you can expect to:
- Stay in the intensive care unit (ICU) for 3 – 5 days. The medical team will closely monitor your condition to watch for signs of complications, and frequently test your liver function.
- Spend 5 – 10 days in the hospital. Once you're stable, you will be taken to a transplant general ward to continue recuperating.
- Have frequent outpatient consultations as you continue recovering at home. You may undergo blood tests a few times each week, which should lessen over time.
- Take immunosuppressant medication for the rest of your life. This is to prevent your immune system from rejecting your new liver.
Care and recovery after a LDLT
After a liver transplant, it is important to care for your new organ, which includes:
- Adopting a healthy lifestyle
- Regular exercise
- Healthy diet
- Taking medication
- Going for follow-up medical appointments regularly
Your transplant coordinators, dietitians and allied healthcare team will educate and guide you on your post-transplant care.
Outpatient check-ups
Organ transplants have the highest risk of organ rejection within the first 60 days after the transplant:
- For the first 2 months, you may need to attend weekly clinical reviews.
- After the first 2 months, the frequency of visits will be adjusted based on your recovery performance.
Immunosuppression (anti-rejection) medicine
After your liver transplant, you will be prescribed immunosuppressants to stop the immune system from rejecting the new liver. You will need to take them daily for the rest of your life.
The daily dosage is carefully calculated by your transplant physician. It is not recommended to make adjustments to your medication before consulting your doctors, as it may lead to organ rejection.
Immunosuppressants will also increase your vulnerability to infections, especially in the first few months after the transplant when higher doses of these medications are typically required.
Your risk decreases slowly as the drug doses are reduced in the months after. However, you need to be mindful at all times to:
- Avoid contact with individuals with infection
- Avoid eating any raw foods
- Get treated immediately if you experience any signs of infection
While you are on anti-rejection medications you should also:
- Avoid certain foods, such as pomelo and grapefruit, as these can affect the effectiveness of the immunosuppressants.
- Inform your doctor before taking any new medications, including over-the-counter medications and supplements, as these may interact with your immunosuppression and alter their effectiveness.
- Inform any healthcare personnel that you are taking anti-rejection medication before undergoing any dental or medical procedure.
Recognising organ rejection and infection
While anti-rejection medication helps prevent organ rejection, it may still occur. This condition can, however, be reversed if the signs are discovered and treated early.
Symptoms and signs of liver rejection include:
- Fever
- Dark, tea-coloured urine
- Jaundice (yellowish skin and eyes)
- Pale or clay–coloured stools
- Chills, aches, unexpected tiredness and abdominal discomfort
Other than the risk of organ rejection, you will also need to be alert about infection, especially since immunosuppressants will reduce your body’s ability to fight infection.
You can minimise your risk of an infection by:
- Practising good personal hygiene.
- Taking precautions to reduce the risk of getting an infection; for example, avoiding crowded places especially during the cold or flu season.
- Washing your hands often.
Contact your transplant coordinator if any of the below signs occur:
- Fever
- Redness or white spots on the tongue or in the mouth
- Redness, swelling or foul-smelling discharge on open wounds
- Persistent cough without shortness of breath
- Flu-like symptoms
- Painful or burning sensation when passing urine
- Diarrhoea
Nutrition after liver transplant
A dietitian will advise you on maintaining a healthy, balanced diet. Depending on your medical condition, you may be placed on a special diet.
It is important for you to maintain a healthy weight, as weight gain and obesity can damage your new liver and increase your risk of chronic diseases, such as high blood pressure and heart disease.
With a weakened immune system caused by anti-rejection medication, it is important to practise safe food handling. The dietitian and nurses will advise you on how to handle food safely and what foods to take note of.
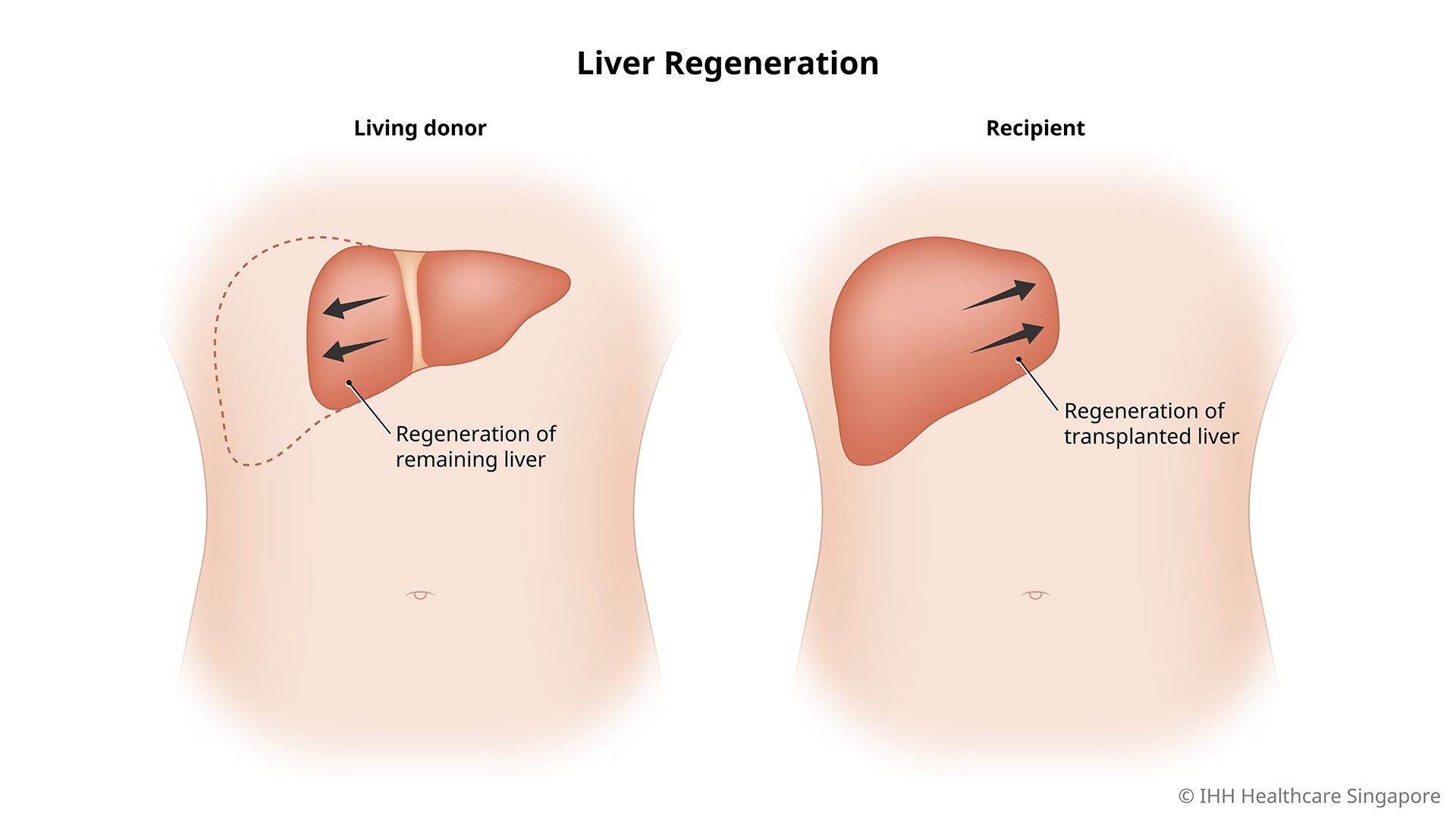
Recovery period for an LDLT
It may take 3 – 6 months to fully recover from your liver transplant surgery.
Most liver transplant recipients are able to resume normal activities or go back to work a few months after surgery, depending on how ill they were before their liver transplant.
Resuming regular activities after your transplant
Before you resume your regular activities, take note of the following:
- Exercise – You may resume exercise to maintain your weight and physical health. However, you should avoid driving for up to 6 weeks after your transplant. For at least 2 months after your surgery, avoid activities that strain your stomach, including heavy lifting and sit-ups.
- Sun exposure – Transplant patients have a chance of developing skin cancer when exposed to the sun. Use sunblock with at least SPF 30, and wear long-sleeved shirts and a hat when outdoors. You should also examine your skin regularly for abnormal growths or patches.
- Travel – Unless you are returning to your own country, you should avoid travelling within the first 6 months after your liver transplant. Your transplant coordinator will also advise you on which areas to avoid, as some countries may pose a higher risk of infection for liver transplant patients.

 Brain & Spine Care
Brain & Spine Care